Home » Cancer Types » Lymphoma
Lymphoma
- Overview
- Treatment Options
- What to Expect
Facts About Lymphoma
The lymphatic system is a network of tiny vessels extending throughout the body. They are often next to the veins and arteries but are even smaller than them. Scattered along these vessels are lymph nodes. The lymphatic vessels carry a clear fluid called lymph from the extremities and organs back to the blood circulation. The job of the lymphatic system is to fight infection and disease. Cancer of the lymphatic system is called lymphoma. The two main types are Hodgkin’s and non-Hodgkin’s lymphomas.
Hodgkin’s Lymphoma
- Hodgkin’s lymphoma (or Hodgkin’s disease) most often begins in the larger, more central lymph nodes of the body 0 those along the largest blood vessels of the neck, central chest, abdomen along the spine, and armpit and groin areas where the vessels return from the arms and legs.
- It is names for the British doctor Thomas Hodgkin, who first described the disease in 1832.
- According to the American Cancer Society, more than 8,000 people will be diagnosed with Hodgkin’s in the United States each year.
- Hodgkin’s is very treatable and often curable. More than 75 percent of patients with Hodgkin’s live longer than 10 years after diagnosis.
- Hodgkin’s is usually treated with radiation therapy and/or chemotherapy, either alone or together.
Non-Hodgkin’s Lymphoma (NHL)
- NHL is a cancerous growth of cells that make up the lymph nodes.
- NHL is eight times more common than Hodgkin’s lymphoma. The American Cancer Society expects that 63,000 people will be diagnosed with the disease annually.
- Since the 1970s, the number of people with NHL has increased significantly. Researchers are studying to see whether a gene makes people more likely to develop NHL.
- There are about 30 types of NHL, and the best treatment depends on the exact type. All types of NHL are treatable, and many are curable.
- NHL is usually treated with chemotherapy, radiation therapy, biologic therapy and/or a stem cell transplant. Depending on your cancer and overall health, you might receive only one of these treatments or several in combination.
Staging of Lymphoma
The stage of lymphoma is a term used to describe the extent of the disease.
- Stage I: Single lymph node or non-lymph node region is affected.
- Stage II: Two or more lymph nodes or non-lymph node regions are affected on the same side of the diaphragm (the muscle under the lungs).
- Stage III: Lymph nodes or non-lymph node regions above and below the diaphragm are affected.
- Stage IV: The cancer has spread outside the lymph nodes to organs such as the liver, bones or lungs. Stage IV can also refer to a tumor in another organ and/or tumors in the distant lymph nodes.
Talk to your physician to find out exactly which stage you have. Determining the stage and exact type of lymphoma (by microscopic examination of tissue from a biopsy) are essential steps toward planning the best treatment to cure your disease.
Treatment Options for Lymphoma
Treatment options depend on the type of lymphoma, its stage and your overall health. Treatment may include chemotherapy or radiation therapy, either alone or in combination. It may help to talk to several specialists before deciding on the best course of treatment for you, your disease and your lifestyle.
- A radiation oncologist is a doctor who specializes in destroying diseased cells with high-energy X-rays or other types of radiation.
- A medical oncologist is a doctor who is an expert at prescribing special drugs (chemotherapy) to treat disease. Some medical oncologists are also hematologists, meaning they have experience treating drug disorders.
Understanding Radiation Therapy
Radiation therapy, also called radiotherapy, is the careful use of radiation to kill diseased cells safely and effectively while avoiding nearby healthy tissue.
- Radiation oncologists use radiation therapy to cure disease, to control disease growth or to relieve symptoms, such as pain.
- Radiation therapy works within diseased cells by damaging their ability to grow. When these cells are destroyed by the radiation, the body naturally eliminates them.
- Healthy tissue can also be affected by radiation, but they are usually able to repair themselves in a way that cancer cells cannot.
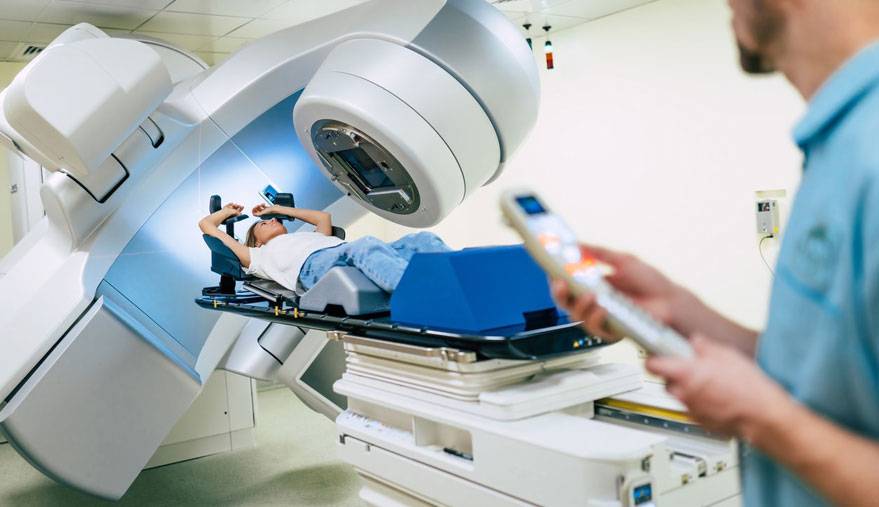
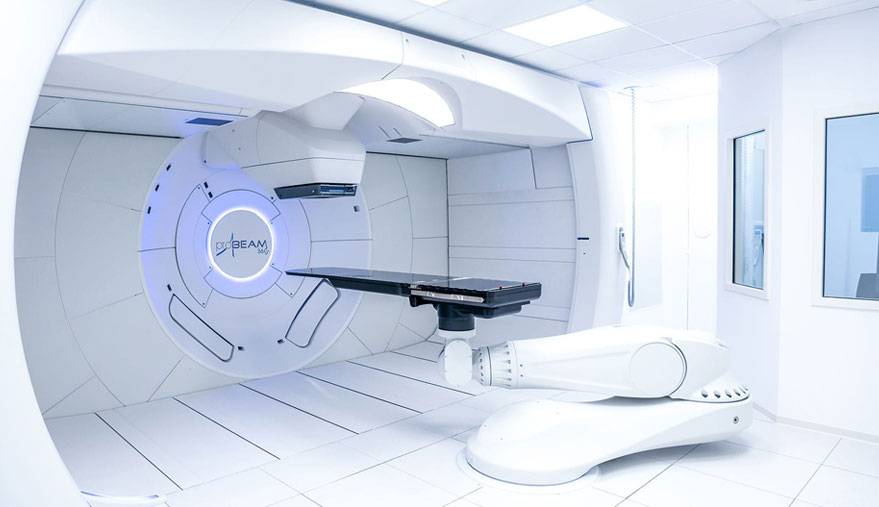
External Beam Radiation Therapy
External beam radiation therapy is a series of outpatient treatments to deliver radiation to the diseased cells accurately. Radiation therapy has been proven to be very successful at treating and curing lymphoma.
- Radiation oncologists deliver external beam radiation therapy to the lymphoma from a machine called a linear accelerator.
- Each treatment is painless and is similar to getting an X-ray. Treatments last less than 30 minutes each, every day but Saturday and Sunday, for several weeks.
- Involved field radiation is when your doctor delivers radiation only to the parts of your body known to have the disease. It is often combined with chemotherapy. Radiation above the diaphragm to the neck, chest and/or underarms is called mantle field radiation. Treatment below the diaphragm to the abdomen, spleen and/or pelvis is called inverted-Y field radiation.
- Your radiation oncologist may deliver radiation to all the lymph nodes in the body to destroy cells that may have spread to other lymph nodes. This is called total nodal irradiation.
- Your radiation oncologist may also deliver radiation to the entire body. This is called total body irradiation. It is often done before chemotherapy and a stem cell or bone marrow transplant to eliminate any diseased cells.
Radiation therapy may be used alone or in combination with chemotherapy or biologic therapy. You will work with your radiation oncologist to agree on a treatment plan that is best for you.
Biologic Therapy
Also called immunotherapy, biologic therapy works with your immune system to fight disease. Biologic therapy is like chemotherapy. The difference is that chemotherapy attacks the diseased cells directly, and biologic therapy helps your immune system fight the disease.
- Monoclonal antibodies work by targeting certain molecules in the body and attaching themselves to those molecules. This causes some cells to die and makes others more likely to be destroyed by radiation and chemotherapy.
- Radiolabeled antibodies are monoclonal antibodies with radioactive particles attached. These antibodies are designed to attach themselves directly to the diseased cells and damage them with small amounts of radiation without injuring nearby healthy tissue.
Effective, safe and compassionate patient care is our top priority
Possible Side Effects
The side effects you might experience will depend on the part of the body being treated, the dose of radiation given and whether you also receive chemotherapy. Before treatment begins, ask you doctor about possible side effects and how best to manage them.
- You may experience mild skin irritation like a sunburn, sore throat or upset stomach, loose bowels movement and/or fatigue. Most side effects will go away when treatment ends.
- Radiation to your head or mouth may cause mouth dryness that can lead to tooth decay. Fluoride treatments may help, so your radiation oncologist will ask you to see a dentist before treatment begins.
- You might loose you hair in areas treated. Your hair will grow back, but it might not have the same texture or thickness.
- Tell your doctor or nurse if you experience any discomfort. They may be able to prescribe medication or change your diet to help.
These side effects are temporary and should go away after treatment ends. Your doctor will discuss any possible long-term side effects with you before treatment begins.
Effective, safe and compassionate patient care is our top priority
Latest News
Dr. Lonika Majithia publishes on The Clinical Utility of DCISionRT on Radiation Therapy Decision Making in Patients with Ductal Carcinoma In Situ Following Breast-Conserving Surgery in Annals of Surgical Oncology
Abstract Background The role of radiation therapy (RT) following breast-conserving surgery (BCS) in ductal carcinoma in situ (DCIS) remains controversial. Trials have not identified a low-risk cohort, based on clinicopathologic features, who do not benefit from RT. A biosignature (DCISionRT®) that evaluates recurrence risk has been developed and validated. We evaluated the impact of DCISionRT […]
Dr. Avani Rao publishes on plan quality effects of proton therapy for central nervous system and skull base tumors in Radiotherapy and Oncology
Abstract Purpose With reports of CNS toxicity in patients treated with proton therapy at doses lower than would be expected based on photon data, it has been proposed that heavy monitor unit (MU) weighting of pencil beam scanning (PBS) proton therapy spots may potentially increase the risk of toxicity. We evaluated the impact of maximum […]
Dr. Daniel Kim publishes on the implications of practice consolidation among radiation oncologists
Abstract Purpose Health care practices across the United States have been consolidating in response to various market forces. The degree of practice consolidation varies widely across specialties but has not been well studied within radiation oncology. This study used Medicare data to characterize the extent of practice consolidation among radiation oncologists and to investigate associated […]
Cancer Types
Radiation Oncology Associates is the leader in comprehensive and cutting-edge radiation oncology therapy services in convenient and accessible locations across Northern Virginia.