Home » Cancer Types » Head & Neck Cancer
Head & Neck Cancer
- Overview
- Treatment Options
- What to Expect
Treatment for head and neck cancer depends on several factors, including the type of cancer, its size and stage, its location and your overall health. Surgery, radiation therapy and chemotherapy are the mainstays of treating head and neck cancers.
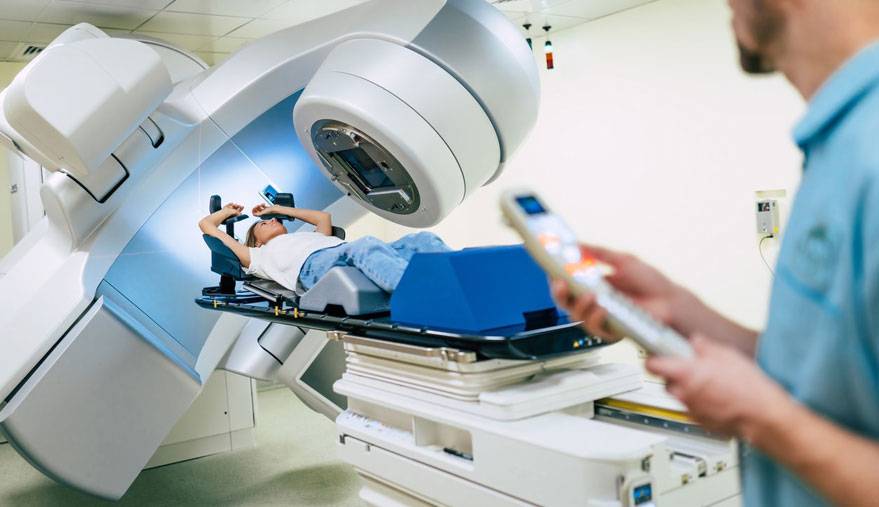
Doctors Bajaj, Chapman, Gao, and Johnson have particular interest and expertise in the treatment of head and neck cancers with advanced radiation technologies including proton therapy and intensity modulated radiation therapy (IMRT). Our cutting-edge technologies allow us to maximize the chance of cure while minimizing treatment related side effects. We strive to provide our patients with the most comprehensive, multidisciplinary care for head and neck cancers working with a highly skilled team comprised of:
- Radiation Oncologists
- Medical Oncologists (Chemotherapy Doctors)
- Otolaryngologists (ENT Doctors)
- Speech & Language Pathologists
- Radiologists and Nuclear Medicine Physicians
- Gastroenterologists
- Dental Oncologists
- Nutritionists and Dieticians
- Oncology Nurses
- Social Workers
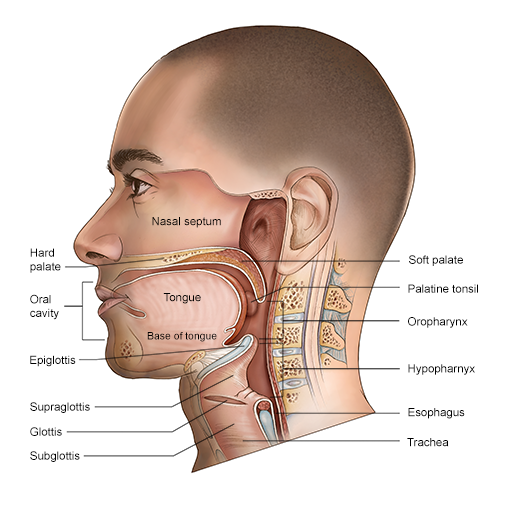
For many head and neck cancers, combining two or three types of treatments may be most effective. That’s why it is important to talk with several cancer specialists about your care, including a surgeon, a radiation oncologist and a medical oncologist. We emphasize a multidisciplinary approach in order to determine the optimal treatment strategy for each patient.
Radiation therapy treatments are delivered in a series of painless daily sessions. Treatments are usually scheduled Monday through Friday, for five to eight weeks. However, your radiation oncologist may schedule your treatments more or less often depending on your cancer.
3D-CRT
Three-dimensional conformal radiotherapy (3D-CRT) combines multiple radiation treatment fields to deliver precise doses of radiation to the affected area.
IMRT:
Intensity modulated radiation therapy (IMRT) is a form of 3D-CRT that further modifies the radiation by varying the intensity of each radiation beam. This allows a precise adjustment of radiation doses to the tissue within the target area with the added advantage of daily image guidance (IGRT). Your ROA physician will discuss if these approaches to therapy are suitable in your case.
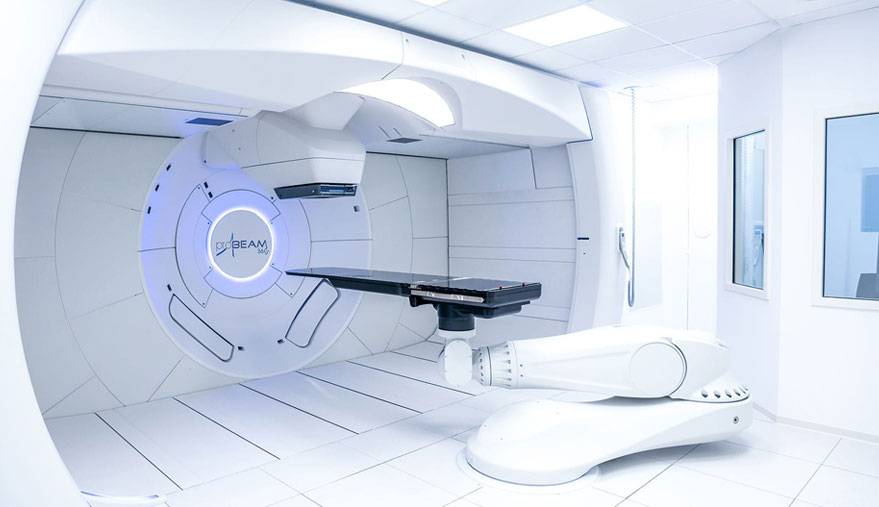
Proton Therapy:
Proton therapy is a highly advanced form of radiation therapy that treats tumors with high precision, conforming to the shape of the tumor and reducing the risk of side effects and damage to surrounding healthy tissues. Unlike photon based treatments, protons have the unique property of delivering the majority of their energy or “dose” directly in the tumor, without going beyond it, into normal tissues. This special behavior allows tumors to receive more targeted doses, while reducing damage to the healthy tissues that surround the tumor, decreasing side effects including damage to your salivary glands.
Different tumors benefit from different treatment technologies. Your doctor will work with you to determine which treatment modality is optimal for your care.
Effective, safe and compassionate patient care is our top priority
To help you keep still during treatment, your doctor may use a plastic mask over your head and shoulders. This device has holes so you can see and breathe through it, is specially designed to fit snugly on you. Wearing the mask doesn’t hurt.
Possible Side Effects
- Side effects of radiation therapy are limited to the area that is receiving treatment.
- Side effects can include redness of the skin, sore mouth and throat, dry mouth, thick phlegm, alteration of taste, pain on swallowing and hair loss on your head, neck and face. Fatigue, or feeling tired, is also very common.
- The way foods taste and the amount of saliva you produce should improve after treatment ends. However, foods may never taste exactly as they did before treatment.
- Side effects are different for each patient. Medications may be prescribed to make you as comfortable as possible. Nutritional supplements may be given to help prevent weight loss.
- If at any time during your treatment you feel discomfort, tell your doctor or nurse. They can prescribe medicine to help you feel better.
Dental Care During Treatment
- It is very important to take care of your teeth during and after treatment. Radiation therapy to the head and neck area may increase your chances of mouth infections and tooth decay.
- Before staring radiation therapy, see your dentist. He or she will also want to see you during your treatment to help you care for your mouth.
- Careful brushing of your teeth can help prevent tooth decay, gum disease and jaw infections. Use a fluoride toothpaste without abrasives.
- Floss gently between your teeth daily using waxed, non-shredding dental floss.
- It may help to rinse daily with a salt and baking soda solution.
- Your dentist may suggest applying fluoride to your teeth regularly.
- Treat the skin exposed to radiation with special care. Stay out of the sun, avoid hot or cold packs, only use lotions on your skin after checking with your doctor or nurse and clean the area with warm water and mild soap. We often have special lotions we can provide for you during your treatment.
- Battling Cancer is tough. Seek out help from support groups and friends.
Effective, safe and compassionate patient care is our top priority
Latest News
Dr. Lonika Majithia publishes on The Clinical Utility of DCISionRT on Radiation Therapy Decision Making in Patients with Ductal Carcinoma In Situ Following Breast-Conserving Surgery in Annals of Surgical Oncology
Abstract Background The role of radiation therapy (RT) following breast-conserving surgery (BCS) in ductal carcinoma in situ (DCIS) remains controversial. Trials have not identified a low-risk cohort, based on clinicopathologic features, who do not benefit from RT. A biosignature (DCISionRT®) that evaluates recurrence risk has been developed and validated. We evaluated the impact of DCISionRT […]
Dr. Avani Rao publishes on plan quality effects of proton therapy for central nervous system and skull base tumors in Radiotherapy and Oncology
Abstract Purpose With reports of CNS toxicity in patients treated with proton therapy at doses lower than would be expected based on photon data, it has been proposed that heavy monitor unit (MU) weighting of pencil beam scanning (PBS) proton therapy spots may potentially increase the risk of toxicity. We evaluated the impact of maximum […]
Dr. Daniel Kim publishes on the implications of practice consolidation among radiation oncologists
Abstract Purpose Health care practices across the United States have been consolidating in response to various market forces. The degree of practice consolidation varies widely across specialties but has not been well studied within radiation oncology. This study used Medicare data to characterize the extent of practice consolidation among radiation oncologists and to investigate associated […]
Cancer Types
Radiation Oncology Associates is the leader in comprehensive and cutting-edge radiation oncology therapy services in convenient and accessible locations across Northern Virginia.